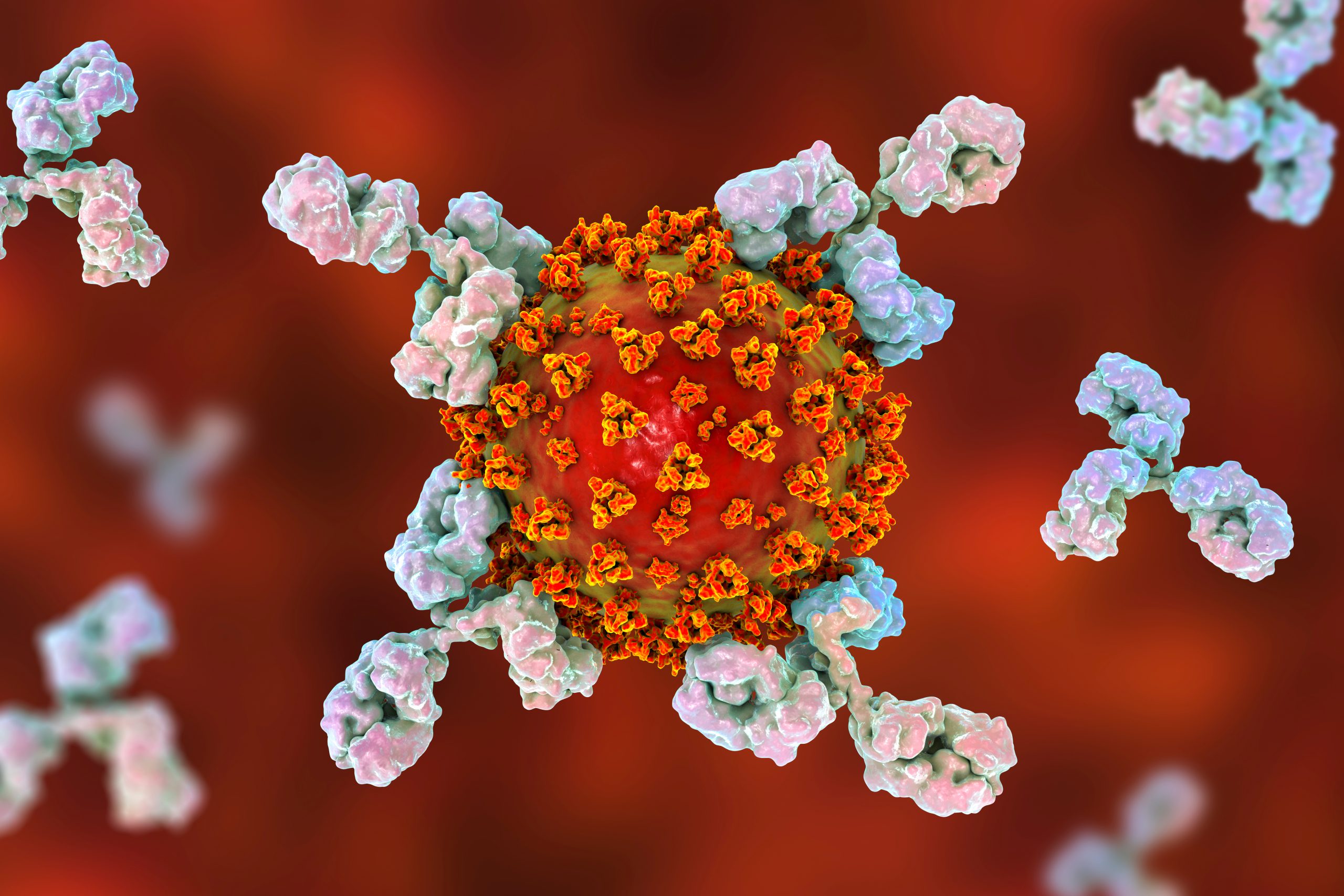
Advancing neutralising antibody therapies for COVID-19
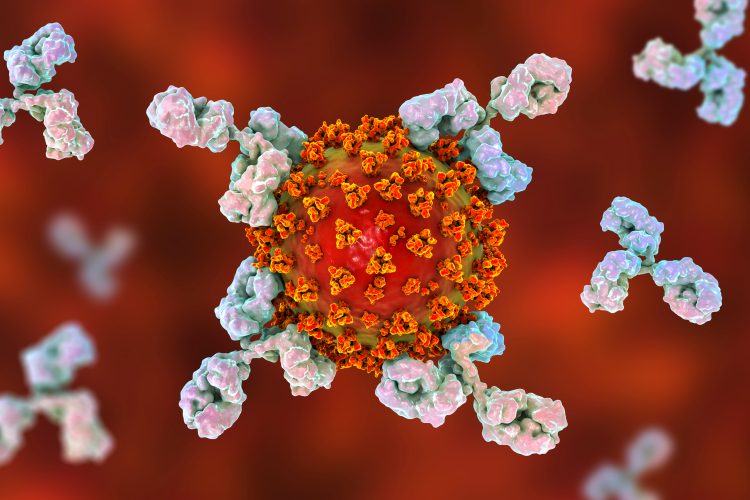
In this article, Ian Chan, Chief Executive Officer and Co-Founder of biotech company Abpro, discusses the development of neutralising antibodies for SARS-CoV-2. Abpro’s neutralising antibody candidate ABP 300 is currently in Phase II/III trials.