Begin with the end in mind: designing synthetic antibiotics with a universal mechanism of action
Posted: 6 May 2020 | Victoria Rees (Drug Target Review) | No comments yet
James Graham from Recce Pharmaceuticals discusses how a new class of synthetic antibiotics could be the key to preventing the spread of antibiotic resistance.
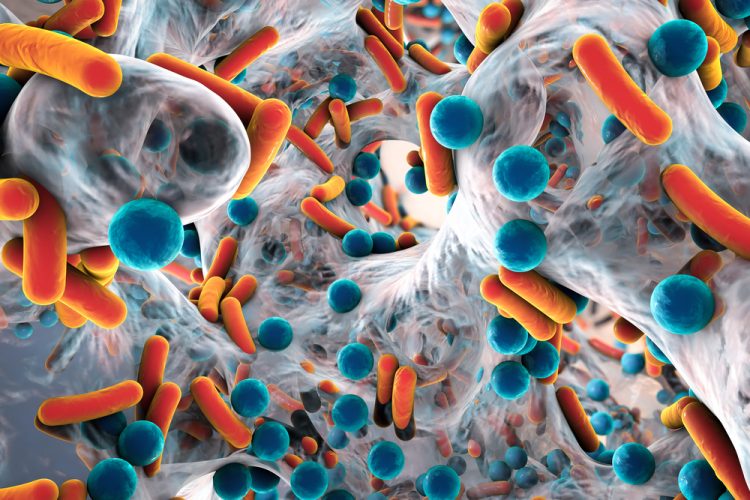

The rising threat of antimicrobial resistance (AMR) is prompting many researchers to investigate potential new antibiotics. Preventing the spread of dangerous bacteria, especially in a hospital environment, could save the lives of many patients who die from conditions such as sepsis.
Drug Target Review’s Victoria Rees spoke to James Graham, Executive Director of Recce Pharmaceuticals, to find out how researchers are attempting to combat harmful bacteria with a novel range of synthetic antibiotics.
The ESKAPE pathogens
A group of the deadliest pathogens are known as the ESKAPE bacteria, which are: Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa and Enterobacter.
Drug Target Review has just announced the launch of its NEW and EXCLUSIVE report examining the evolution of AI and informatics in drug discovery and development.
In this 63 page in-depth report, experts and researchers explore the key benefits of AI and informatics processes, reveal where the challenges lie for the implementation of AI and how they see the use of these technologies streamlining workflows in the future.
Also featured are exclusive interviews with leading scientists from AstraZeneca, Auransa, PolarisQB and Chalmers University of Technology.
Approximately 700,000 people die every year from antibiotic-resistant infections globally – many of these are from the ESKAPE pathogens. Due to their rate of mutation, they pose a significant threat to patients.
Graham highlighted that currently, there are no efficacious antibiotics that tackle the ongoing mutation of the ESKAPE pathogens and thus prevent the spread of resistance. Therefore, when an ESKAPE pathogen enters the bloodstream, especially by way of sepsis, it can prove dangerous for the patient. Graham added that diagnostics are often slow to inform doctors which pathogen has infected a patient and the likelihood of survival decreases by six percent each hour, making these bacteria potentially lethal.
The situation, Graham emphasised, is clear: “Bacteria continue to mutate, but drugs are not keeping up and so doctors and patients are suffering.”
Tackling the pathogens – a novel class of antibiotics

Instead of following the traditional route and using natural products to derive antibiotics from, Graham explained that Recce designed its compound based on what was required from it: “Begin with the end in mind.”
This mindset allowed the researchers to produce a synthetic antibiotic with a unique mechanism of action. Rather than a few active sites, this new class of antibiotics has millions of active sites, said Graham. He explained that this overcomes the issue of AMR as it circumvents the ‘lock-and-key’ mode of action that traditional antibiotics use.
…patients should be able to feel confident when going to the doctor and getting the medicines they require”
According to Graham, the novel antibiotics overcome mutations by taking advantage of elements unique to bacteria; these microorganisms have high metabolic processes within the internal cell – up to 10 atmospheres of pressure. He explained that once RECCE 327 enters the bloodstream, it works by binding to a pathogen’s outer membrane and interacting with the bacterial plasma membrane proteins, which weakens the cell.
“We cause those bacteria to burst and have identified in dozens of studies no concerning inhibition of other healthy cells,” said Graham.
Drug design
Graham explained that the new antibiotics are made from polymers, where certain parts of the chain contain hydrophobic monomers with hydrophobic-attractive coatings.
These typically seek out the bacteria and attempt to bind to the proteinaceous layer of the bacterial cell wall. Once the polymer has successfully sought out the bacteria, the antibacterial properties of the chain can take their effect.

Developing a new compound
One challenge when introducing a new concept in pharmaceuticals is that there is a learning curve and new data, not presently seen and referenceable in scientific literature, said Graham.
Rather than a few active sites, this new class of antibiotics has millions of active sites”
Investigating the compounds meant that the researchers developing RECCE 327 had to seek out new data: “Everybody is doing the same thing as everybody else yet perplexed they kept getting the same answer; not taking that radical step forward. Antibiotic developers are often complaining of baseline market prices; I cannot think of an industry anywhere that will pay a premium for a 30-year-old variant on a theme technology. We aim to given clinicians what they really want and patients the medicine they deserve – that takes some unprecedented innovation.”
Drug development is set of precedent – backward (historical) thinking. That is a challenge when it comes to forward thinking and communication of new, ground-breaking innovation.
What is the next stage for RECCE 327?
According to Graham, this new class of synthetic antibiotics is an entirely new and unique category beyond traditional antibiotics. Thanks to the unique mechanism of action (MoA), they can continue to work with repeated use, which “not only gives patients a new sign of hope , but also re-empowers clinicians to tackle a wide range of unmet medical needs, without fear of bacterial mutation and resistance.”


The company has completed its pre-clinical studies to assess RECCE 327 and will now move onto its first-in-human Phase I trial. This study will be conducted in 40 healthy volunteers to evaluate the drugs’ safety, tolerability, pharmacokinetic and pharmacodynamic properties. The antibiotic will be administered via an intravascular infusion down the pathway of sepsis.
The first patients are expected to be dosed in the second half of 2020 in a randomised, double-blind, placebo-controlled single ascending dose study.
Graham also said that in parallel, at a leading teaching hospital in Australia, he anticipates a topical efficacy trial to assess its success on bacterial wounds, assisting in wound closure by removing the bacterial burden around the wound site, skin infections and burns.
Conclusion
Graham highlighted the irony that the antibiotic pipeline has never been dryer, despite “the need never being greater.”
He said that in the coming years, patients should be able to feel confident when going to the doctor and getting the medicines they require – a future in which RECCE 327 could play a crucial role.
“In the context of supporting the antibiotic stewardship model by that unique mechanism of action and inability to fail with repeated use, we ultimately complement all interested parties in the process,” concluded Graham.
Related topics
Antibiotics, Antimicrobials, Drug Development, Drug Targets, Research & Development
Related conditions
Sepsis
Related organisations
Recce Pharmaceuticals
Related people
James Graham



